Introduction
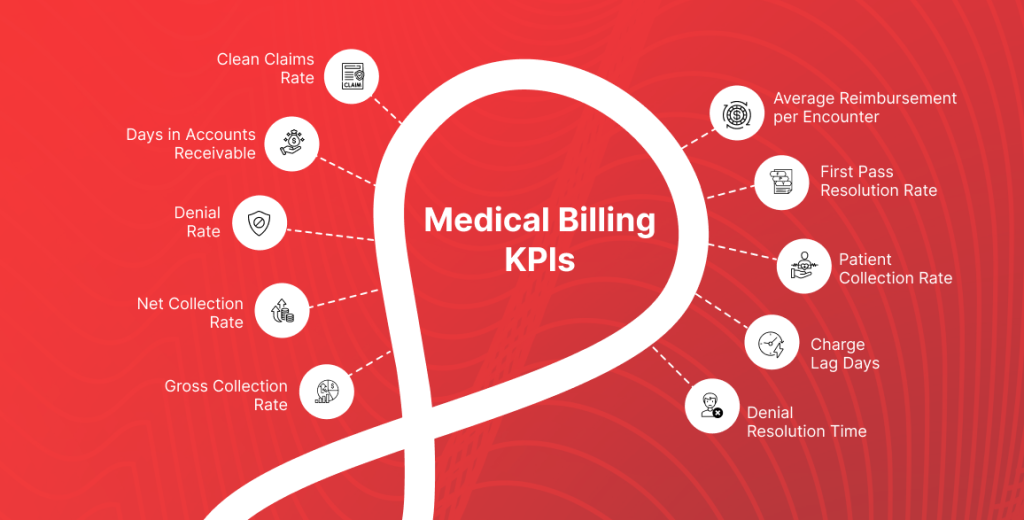
The healthcare industry is changing quickly. Today, the financial health of a practice is determined not only by the number of patients but also by the efficiency of revenue cycle management. With the transformation in medical billing, including payer guidelines, updates to coding, and increasing patient responsibility, monitoring KPIs (key performance indicators) has become more important than ever. The Clean Claim Rate, Denial Rate, First Pass Resolution Rate, and Net Collection Rate help practices measure claim accuracy, rejection frequency, first-submission success, and the percentage of revenue actually collected. Implementing an effective KPI strategy for your revenue cycle will result in a decrease in claim denials, shorter reimbursement times, and a more stable cash flow. Therefore, KPIs provide your practice with the ability to convert raw billing data into usable information to better help you expand and ensure long-term growth.
Why Medical Billing KPIs Matter
The Revenue Cycle Management process includes all financial transactions that a patient has with a provider and ranges from when they schedule their visit until final payment is made. Every step in the revenue cycle process can lead to miscalculations, delays or loss of revenue for that provider. If these problems are not tracked, they generally go undiscovered until they begin to significantly hurt the provider’s financial performance. Therefore, it is critical for today’s healthcare providers to measure KPIs during revenue cycle management processes. Industry research shows that providers who continuously measure and improve their RCM KPIs can improve their collection rates by as much as 20% and lower their denial rates compared to others in the industry.

Clean Claims Rate (CCR)
The clean claim rate is one of the most essential measures of billing effectiveness. This metric measures the percentage of claims submitted accurately and accepted as valid by the payer at first submission, without being corrected or resubmitted. Most consider 95% or above to be a good benchmark and indicates that the front end was well executed (good patient registration, verification of insurance and accurate coding). When the clean claim rate is below this benchmark, it typically indicates there are systemic reasons for delays, as well as higher costs associated with administrative work.
For example, a small internal medicine clinic with a history of claim rejections decided to implement an automated claim scrubbing system, which would allow them to identify errors in submitted claims before submitting them. The claims were researched for compliance with payer requirements. After implementing the scrubbing system and making corrections to previously submitted claims, the clean claim rate improved from 88% to 96%, resulting in quicker payments and better operational efficiency. This illustrates how an improvement in this KPI can have a substantial positive effect on revenue cycle management.
Days in Accounts Receivable(A/R)
How quickly a practice is able to receive payments after providing services can significantly impact the financial health of that practice. The number of days a claim stays open, i.e., unpaid, as measured by A/R days is an important metric in assessing how well an organization is being able to collect payments in a timely manner following the services rendered. The average days in A/R for an organization should fall within a range of approximately 30-40 days. If the days in A/R for an organization are higher than this range it results in a delay in receiving payment, which in turn negatively impacts the organization’s cash flow and creates financial instability for the organization.

For example, an organization that offers cardiology practice was facing a late payment issue. It later decided to outsource its A/R management to an RCM service provider. Resultantly, it reduced its A/R days from 52 days to 34 days. This reduction in days in A/R helped improve the cash flow and allowed the practice to invest in its patients and its overall operations. Therefore, keeping track of the days in A/R and optimizing that number is critical to the financial health of an organization as well as receiving revenue in a timely manner.
Denial Rate
Claims denial indicates a claim rejection by a payer; hence, it is a key revenue cycle efficiency measure. The general expectation for denial percentage is to be less than 5 to 10 percent; therefore, a higher percentage of denied claims indicates issues with coding, documentation completion, or eligibility verification. Denied claims have negative impacts on both cash flow and work volume for the staff. Denial rate can be minimized by analyzing denied claim patterns (e.g., using a software program) and addressing the root cause(s) of denials.
Net Collection Rate (NCR)
Essentially, the Net Collection Rate is used to evaluate how well a practice collects the revenue it has been contracted to receive after accounting for any adjustments, such as payer discounts. If a practice has an NCR above 95%, it is generally believed that the practice is good at managing collections and minimizing revenue loss. Conversely, if a practice has a low NCR, it may be indicative of issues such as poor follow-up on unpaid claims, underpayments from payors, or ineffective billing processes.
For example, one multi-specialty practice found that a portion of the revenue it expected to collect from payors was being lost because of underpayments that were overlooked by the practice. After implementing a structured follow-up process and utilizing analytics to monitor and audit payment discrepancies, the practice was able to increase its NCR significantly. Due to its significant role in financial performance, it is considered one of the most important KPIs for any practice that is looking to maximize revenue cycle results.
Gross Collection Rate (GCR)
The gross collection rate is an overall indication of how well a practice can collect payments compared to the total amount of charges billed. While it does not include collections from contract adjustments, it allows the practice to have a high-level view of the overall billing efficiency of the practice. A GCR between 85% – 95% is considered to be within the normal range because it contains amounts that may never be recoverable due to payer agreements.
Practices that routinely review their gross collection rate will be able to identify trends in revenue growth and identify potential issues in their billing process. For example, an abrupt drop in the GCR may imply that claims are being increasingly rejected or that payments are being delayed. By reviewing such trends, practices can implement corrective measures to ensure a steady flow of revenue into their practice.

FPRR (First Pass Resolution Rate)
First Pass Resolution Rate measures the percentage of claims that are completed with regard to processing and timely payment. FPRR, as a key performance indicator (KPI), is directly associated with both clean claim rate and denial rate; as such, FPRR provides insight into the overall efficiency of the billing process. High FPRR has traditionally been defined as being greater than eighty-five percent (>85%), which denotes that claims are being submitted correctly and processed seamlessly by payers.
Patient Collection Rate
As patients are required to pay more of their medical costs due to high-deductible health plans and the increase in patient responsibility for out-of-pocket costs, patient collections rates have become a very important metric for determining how well a practice collects from the patient for co-pays, deductibles, and outstanding balances. The proportion of total revenue generated by patient payments is a significant component of healthcare facilities’ overall revenues. Therefore, practices should optimize their collection practices to increase total practice revenue.
Average Reimbursement per Encounter
Average Reimbursement Per Encounter (KPI) enables you to know how much revenue is generated during each patient visit. This provides insight into the accuracy of billing and the performance of your payers. Average reimbursement per encounter is a KPI that can be utilized to determine issues such as mismatched coding, missed charges, or unfavorable payer contracts. For example, an orthopedic clinic completed an audit of its billing procedures and discovered that there were many instances of coding done incorrectly. When the clinic corrected the coding and updated it, it raised its average reimbursement by 15%. By monitoring their Average reimbursement per encounter KPI, practices can be assured that they are capturing the total value of their services and maximizing their revenue opportunities.
Charge Lag Days
Charge-lag-days is an indicator of the duration of time between providing services and submitting claims related to those services for reimbursement. As a target, you want your lag days to be as short as possible (1-3 days). Delays in the entry of charges will significantly slow down the revenue cycle, delay reimbursement, and impact cash flow.

For instance, one department at a hospital has documentation and coding delays that caused it to have a days-lag of more than a week; thus, there were delayed payments received. By improving the workflow between the clinical and billing departments, this department was able to decrease its days lag charge and expedite collection of its revenue.
Denial Resolution Time
The time to resolve denial shows you how quickly denied claims are reviewed/revised/resubmitted for payment. This is a very important metric for getting back lost income due to denied claims, helping reduce overall financial shock. High-performing organizations typically resolve denied claims in 7 to 10 days so that they do not experience delays in receiving payments.
One example is a healthcare organization that created a team solely focused on resolving rejected claims; this led to a great deal of improvement in resolution times and overall increased collections. This will allow the practice to make sure they are addressing their denied claims as quickly as possible and not letting them become a permanent loss of revenue.
Common Mistakes Practices Make
KPIs are important, but many different types do not capitalize on them due to common errors, such as implementing metrics without any analysis of the trend or any type of remedial action. Many practices try to focus on too many KPIs at one time, creating uncertainty and confusion. Multiple KPIs can also be used to demonstrate an ongoing issue (for example, denials) that requires re-examination before they create a remaining problem that influences their revenue. Internal communications between the clinical side of practice and the billing department create an additional common barrier to successfully using KPIs in a manner that will maximize their effectiveness (e.g., improper documentation and/or incorrect coding). Practices need to be committed to a data-driven continuous improvement/re-engineering strategy for implementing KPIs to maximize the value of KPI tracking.
How to Improve Revenue Cycle Performance
For an organization to enhance the performance of its revenue cycle, it requires a combination of technology, labor skill, and proactive management behavior, allowing them to perform respective roles successfully. Automating the processes of verifying insurance eligibility, submitting claims, and tracking payment postings reduces the number of errors made in performing those duties and increases the speed at which each task can be completed. By conducting regular audits, organizations can find inaccuracies in coding or compliance, while continuously providing education to their employees will enable them to stay up to date on current developments in their industry. Organizations also outsource a lot of their RCM responsibilities to companies that specialize in those services and have the expertise as well as the ability to provide both high levels of service quality and efficiency. Finally, if organizations use these strategies together with an effective process of measuring KPIs, they can achieve significant improvements in both their financial and operational performance.
Final Thoughts
Tracking and optimizing medical billing KPIs is essential for any healthcare practice aiming to strengthen financial performance and streamline operations. These RCM metrics offer clear visibility into each stage of the revenue cycle, helping practices uncover inefficiencies, minimize denials, and accelerate reimbursements. By consistently monitoring the right indicators and taking timely corrective actions, healthcare providers can improve cash flow, enhance operational efficiency, and build a more stable and profitable practice.
If you are looking for how medical billing KPIs can be achieved successfully, Onfinio provides the solution with proven efficiency, a strong track record, and data-driven expertise. From accurate claim management to proactive denial reduction and performance tracking, Onfinio ensures your revenue cycle operates smoothly while maximizing your financial outcomes.